In this article 
View / Download
pdf version of this article
Antibiotic use is increasing in New Zealand and around the world. Many patients expect that antibiotics will be
prescribed to them for a variety of respiratory symptoms, including the common cold. This is despite the fact that the
common cold is caused by a rhinovirus and in most cases antimicrobial agents are not needed.1 Cochrane reviews
of research have also found that antibiotics usually have minimal or no benefit when used for sore throat, acute otitis
media, streptococcal tonsillitis and acute purulent sinusitis.2
Although the majority of GPs are aware that antibiotics have limited effectiveness for many upper respiratory tract
infections, they may often still prescribe antibiotics for these conditions due to patient expectation or demand and their
own perception of what the patient wants.3 However the consequences of antibiotic overuse include unnecessary
adverse effects, increased costs and the development of bacterial resistance, which is arguably the most detrimental effect.
An effective strategy for decreasing prescribing of unnecessary antibiotics, without damaging the patient-doctor relationship,
is to give a delayed or back-pocket prescription, to be filled at a later time if the patient's condition does not improve.
A recent study reported that 50% of patients given delayed prescriptions did not fill them.4 Delayed prescribing
also enables GPs to practice more patient-centred medicine by educating patients to take more responsibility for their
own health care management. It also assists the GP in dealing with pressure they may experience from patients expecting
antibiotics, by giving them something to take home and preventing them from visiting another GP to obtain a prescription.5 However,
more work is needed in developing uniform guidelines on when delayed prescriptions are most appropriate.
Education campaigns, targeting both the general public and health care professionals, are one of the most important
tools in reducing unwarranted prescription of antibiotics. PHARMAC launched a campaign in 1999 (‘Wise Use of Antibiotics’)
in response to the growing volume of antibiotics being prescribed in New Zealand. Following this campaign, there was a
national reduction in antibiotic use, attributed in part to changes in the behaviour of both doctors and patients.6
In July 2006, bpacnz produced and distributed an education programme to promote appropriate antibiotic treatment of respiratory
tract infections and to reduce the prescription of antibiotics for viral infections. In order to evaluate the effectiveness
and impact of this campaign, two groups of GPs were randomly selected and asked to participate in a ‘Before/After’ quiz
or a ‘Remembering’ study.
“Before/After Quiz”
One month before the bpacnz campaign was released, a random sample of 150 GPs were contacted by email and asked to complete
a web-based questionnaire testing their knowledge of antibiotic treatment of upper respiratory tract infections. The questionnaire
contained eight clinical scenarios which the GP was asked to consider and then indicate which antibiotic they would prescribe
– amoxicillin, amoxicillin-clavulanate, erythromycin, penicillin V or no antibiotic. Seventy-five percent of GPs (112)
completed the quiz, with an average test score of 3.8 out of 8 (range 1-8). Several patterns emerged such as selecting
amoxicillin-clavulanate where amoxicillin was considered more appropriate and indicating an antibiotic would be given
when antibiotics were not deemed necessary.
One month after the campaign had concluded, the 112 GPs who participated in the “Before Quiz”, along with
an additional randomly selected group of 150 GPs were asked to complete the quiz. The response rate was 59% (76 of the
original GPs and 78 of the new group). The average quiz score after the campaign was 5.5 out of 8 (range 2-8). This was
a significant (p = 0.01) increase in score. There was no significant difference between the two groups.
Although there are several limitations in using this methodology, it can be considered that the bpacnz campaign increased
GPs knowledge of the antibiotic treatment of respiratory infections. It is anticipated that this may result in a decrease
in the volume of antibiotics being prescribed by these GPs.
| Before Quiz |
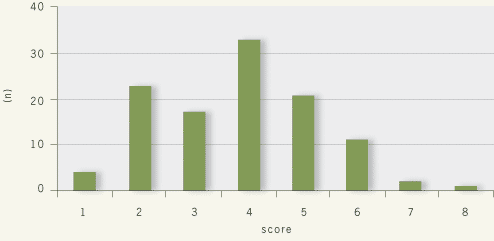 |
| After Quiz |
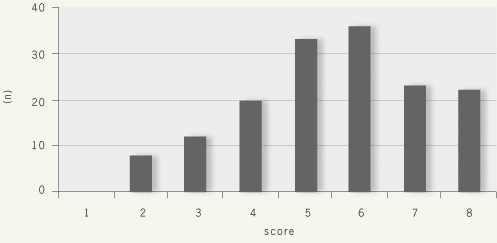 |
‘Remembering’ study
A web based questionnaire surveying GPs on their recollection of the bpacnz Respiratory Infections campaign and subsequent
changes they made to their clinical practice, was emailed to a random sample of 200 doctors, one month after the conclusion
of the campaign. 76 of the 200 GPs responded.
Remembering key messages of the campaign
- Almost all GPs (92%) remembered at least one key message
- Of those who remembered, 55 (79%) remembered one message and 15 (21%) remembered two or more messages
- The most frequently recalled message was; antibiotics aren’t always necessary and their use should be limited and
doses carefully considered
- Other recalled messages included; antibiotics shouldn't be prescribed for viral infection - many infections are viral
and narrower spectrum antibiotics should be used in preference to broader spectrum antibiotics
Making subsequent changes to clinical practice
- Two thirds of the GPs (66%) made at least one change to their clinical practice as a result of the campaign
- Of those who made changes, 39 (78%) made one change and 11 (22%) made two or more changes
- The most common change was prescribing less broader spectrum and more narrower spectrum antibiotics
- The second most frequent change was reducing use of antibiotics and applying more caution in prescribing. Other changes
included; becoming more aware of the issues surrounding antibiotic use and applying this to practice, changing dose and
duration of treatment to follow recommendations and using 'back-pocket' prescriptions
- The most frequent reason given by those who did not make any changes was ‘already carrying out campaign recommendations’
| ‘The bpacnz campaign has improved my knowledge of treating respiratory infections’ |
 |
The ‘Hygiene Hypothesis’
Is there a link between childhood antibiotic use and asthma?
Evidence is emerging of a possible causal association between the increased use of antibiotics and the increased
prevalence of asthma. Asthma is now the most common chronic disease of childhood. The reasons for the asthma epidemic
are not yet fully known. One hypothesis suggests that infections during infancy may protect against asthma by down-regulating
production of immune response cells (IgE). Protection against microbial exposure by using antibiotics may negate this
effect by increasing the immune response. This is known as the ‘Hygiene Hypothesis’.
Researchers from the University of British Columbia undertook a systematic review and meta-analysis of eight studies
(including two New Zealand studies) which investigated the link between antibiotic use in early infancy and subsequent
development of childhood asthma. Their analysis found that exposure to at least one course of antibiotics in the first
year of life was a risk factor for the development of asthma (OR 2.05; 95% CI 1.41-2.99). However the positive association
was largely seen in the results of retrospective studies. These studies relied on data from parent-completed questionnaires
and it is possible that information was influenced by recall bias, as parents of children with asthma may be more likely
to report an earlier exposure to antibiotics. There is also the issue of confounding by indication i.e. children with
asthma are more likely to suffer from respiratory infections in their infancy, requiring antibiotics. Further research
should focus on antibiotics prescribed for non-respiratory tract indications and validated measures of antibiotic exposure,
to eliminate these confounding factors.
The authors concluded that there is some evidence of a relationship between early antibiotic use and development
of asthma in childhood, however further large-scale, population-based studies are needed to determine whether this
is due to the ‘Hygiene Hypothesis’ of antibiotic exposure or simply due to the fact that children with asthma are more
likely to suffer from early respiratory infections treated with antibiotics.
*The full meta-analysis study is available from:
http://www.chestjournal.org/cgi/content/full/129/3/610
Reference: Marra F, Lynd L, Coombes M, et al. Does antibiotic exposure during infancy
lead to development of asthma?: A systematic review and meta-analysis. Chest 2006;129(3):610-18. |
References
- Herlov-Nielsen H, Permin H. Common-cold risk factors, transmission and treatment. Ugeskr Laeger 2001;163:5643-6.
- Arroll B. Antibiotics for upper respiratory tract infections: an overview of Cochrane reviews. Respir Med 2005;99(3):255-61.
- Cockburn J, Pit S. Prescribing behaviour in clinical practice: patients’ expectations and physicians’ perceptions
pf patients’ expectations - a questionnaire study. BMJ 1997;315(7107):520-23.
- Couchman G, Rascoe T, Forjuoh S. Back-up antibiotic prescriptions for common respiratory symptoms. Patient satisfaction
and fill rates. J Fam Pract 2000;49:907-13.
- Arroll B, Goodyear-Smith F, Thomas D, Kerse N. Delayed antibiotics prescriptions: What are the experiences and attitudes
of physicians and patients? J Fam Pract 2002;51(11):954-59.
- Sung L, Arroll J, Arroll B, et al. Antiobiotic use for upper respiratory tract infections before and after an education
campaign as reported by general practitioners in New Zealand. NZ Med J 2006;119(1233):U1956.